Endothelin
By Matthias Barton and Masashi Yanagisawa
(2011)

Three generations of scientists: Setsuro Ebashi (1922-2006) with his wife, Tomoh Masaki (1934-2020) and Masashi Yanagisawa
Photograph taken in 1988 at Okazaki National Research Institute, Japan, courtesy of Professor Yanagisawa
The Discovery of Endothelin
Already in the 1950s the recognition of the mechanisms controlling arterial vasomotion as an essential component of cardiovascular homeostasis using pharmacological tools became a prominent field in physiology research (Furchgott 1955). Consequently, pharmacological studies in the 1970s by Sir John R. Vane (1927-2004) and Salvador Moncada led to the identification of mechanisms indicating that endogenous vasodilator factors play a role in maintaining vascular tone (Vane 1975 ). Specifically, acetylcholine was found to have profound vasodilator effects as independently reported by both Paul Vanhoutte (1940-2019) and Noboru Toda in the 1970s (Vanhoutte 1974; Toda 1974). By the end of the 1970s, Robert F. Furchgott (1916-2009) - by luck and through an unplanned but successful experiment (Furchgott 1993) - discovered that the mechanism of acetylcholine-mediated vasodilation requires the presence intact endothelial cells through the release a dilator factor. As the identity of this factor was unknown at this point, Furchgott termed the substance EDRF (endothelium-derived relaxing factor). This discovery was published in 1980 (Furchgott & Zawadzki 1980). Both, Sir John Vane and Robert Furchgott received the Nobel Prize in Medicine or Physiology for their discoveries which was awarded to them in 1982 and 1998, respectively. Less than a year after Furchgott's paper was published, de Mey and Vanhoutte reported the release of vasoconstrictor factors from endothelial cells (De Mey & Vanhoutte 1982). The finding of the release of vasoconstrictor substances stimulated further research in this area, and within a few years later the release of a peptidergic vasoconstrictor substances was reported (Hickey et al. 1985, Gillespie et al. 1986, O´Brien et al. 1987). These reports again stimulated researchers in Japan lead by Tomoh Masaki (1934-2020, Emoto et al., 2020) with Masashi Yanagisawa as his graduate student to identify this substance (Masaki 1998), which due to its endothelial cell origin was named "endothelin". The sequences of the gene and the peptide were published in a seminal report (Yanagisawa et al. 1988, Emoto et al. 2020)
The Endothelin System
Shortly after the cloning of endothelins (ETs), which include ET-1, ET-2, and ET-3 (Inoue 1988; Schneider et al. 2008), the cellular targets were identified and cloned. In mammals, two endothelin receptors (ETA and ETB) mediate ET actions (Schneider et al. 2008). Endothelin-1, the biologically most potent and predominant member of the endothelin peptide family, preferably binds to ETA receptors, whereas ETB receptors bind both ET-1 and ET-3. The ETB/ET-3 axis can be regarded as an endogenous "antagonist" system opposing the effects of ETA/ET-1 mediated activities. These include potent vasoconstriction, cell growth, embryonic development, renal functions, neurophysiological functions such as pain signaling, cardiovascular homeostasis, cancer cell growth, endocrine function, inflammation, pulmonary functions such as bronchoconstriction and reproductive system functions, among others.
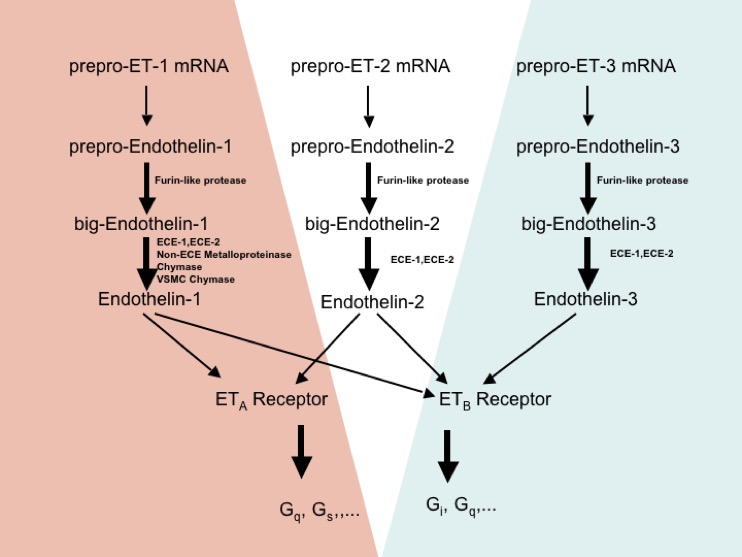
Figure 1: Components of the endothelin system. Prepro-endothelins are formed following transcription and translation from prepro-endothelin mRNA and are subsequently processed by furin-like proteases to form big-ET intermediates that are further cleaved to three physiologically active endothelin peptides by endothelin-converting enzymes and other enzymes. The peptides interact with peptide-selective ETB receptor or non-peptide selective ETA receptors. These receptors couple to G proteins which result in the activation of physiological responses. In red, components of the pre-proET-1 -> ECE-1 -> ET-1 ->ETA receptor axis are shown which is responsible for the development of embryonic cephalic and cardiac neural crest-derived craniofacial and cardiac outflow structures, vasoconstriction, cell growth, and inflammation, among other actions. In blue, the components of the preproET-3 ->ECE-1 ->ET-3 ->ETB receptor axis are shown which is important for the development of neural crest-derived epidermal melanocytes and enteric neurons, natriuresis, and melanocyte growth. Figure reproduced from Can J Physiol Pharmacol 2008; 86: 485-498.
Endothelin in Physiology and Disease
Within a remarkably short time of only 4 years after the discovery of endothelin both its receptors had been cloned and receptor antagonists had become available. The first clinical trial in patients with congestive heart failure was performed in Zurich, Switzerland, in the early 1990s and results were published already in 1995 (Kiowski et al, 1995). Nevertheless, it took several more years and many unsuccessful clinical trials in heart failure patients until the concept of endothelin receptor blockade could be established in clinical medicine. In 2001, bosentan (Tracleer™) was the first orally active endothelin receptor antagonist to receive approval from the U. S. Federal Food and Drug Administration (FDA) for the treatment of patients with primary pulmonary arterial hypertension (PAH) based on convincing evidence of improving clinical status and survival in patients (Davenport 2002). Since, several other endothelin antagonists have become available for the treatment of pulmonary hypertension, including ambrisentan (Letairis™).
Research in the past two decades using endothelin receptor antagonists (ERAs) has resulted in a wealth of information about the role of ET-1 and its receptors in the regulation of biological functions and disease in animal models as well as in humans. Endothelins, of which ET-1 represents the predominant and biologically most relevant isoform (Kedzierski and Yanagisawa 2001), can be considered ubiquitously expressed stress-responsive regulators working in an paracrine and autocrine fashion, with both beneficial and detrimental effects (Kedzierski and Yanagisawa 2001). Endothelins exert a number of physiological functions, including neural crest cell development and neurotransmission (reviewed in Kedzierski and Yanagisawa 2001). In the vascular system, endothelin via activation of ETA receptors has a basal vasoconstricting role and contributes to the development of vascular disease in hypertension and atherosclerosis. Endothelins contribute to myocardial contractility, chronotropy (Kedzierski and Yanagisawa 2001) and arrhythmogenesis, as well as myocardial remodelling following post-infarct congestive heart failure. In the lung, the endothelin system regulates the bronchial tone (Uchida et al. 1988) and proliferation of pulmonary airways blood vessels and promotes the development of pulmonary hypertension. Endothelin also controls water and sodium excretion and acid-base balance in the kidney under physiological conditions (Kohan 2008), and promotes the development of glomerulosclerosis). In the brain, the endothelin system modulates cardio-respiratory centers and release of hormones (Kedzierski and Yanagisawa 2001) and contributes to growth guidance of developing sympathetic neurons. In addition, endothelins affect physiology and pathophysiology of the immune system, in the liver, muscle, bones, skin, in the prostate, in adipose tissue),in the reproductive tract, and are involved in glucose homeostasis.
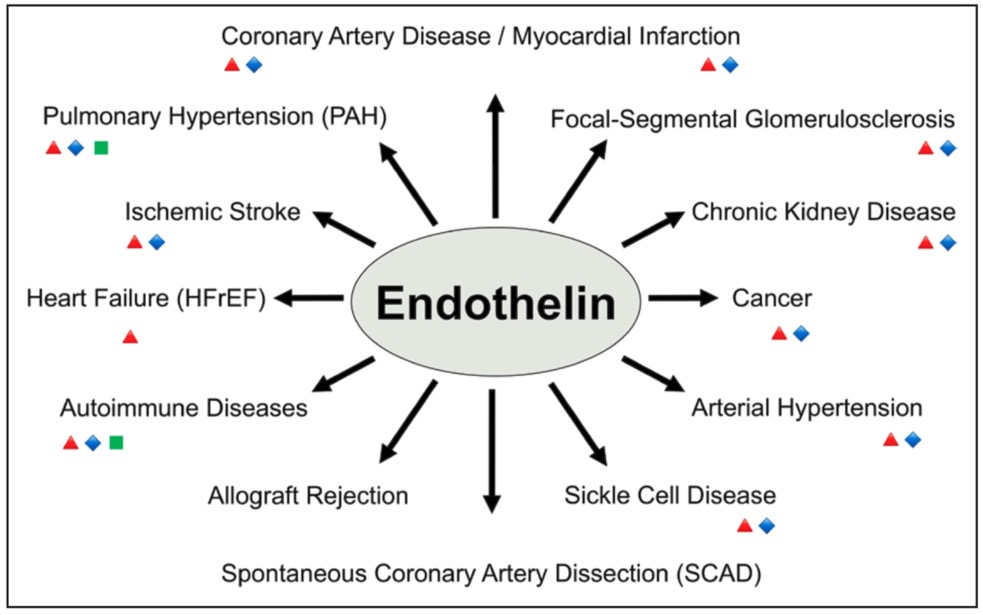
Figure 2: Disease conditions in which the endothelin system has been implicated. Red triangle indicates clinical study, blue diamond indicates therapeutic benefit demonstrated in some clinical studies, and green square indicates regulatory approval of endothelin receptor antagonists for this indication. Autoimmune diseases refer to scleroderma / systemic sclerosis–related digital ulcers. PAH indicates pulmonary arterial hypertension. Figure reproduced from Hypertension 2019; 74: 1232-1265
Endothelin Receptor Antagonists: Current Clinical Perspectives
Thirty years after its discovery it has become clear that endothelin is not merely a vasoconstrictor but that it is a multifunctional peptide with cytokine-like activity which effects almost all aspects of cell function. Although pharmaceutical companies set out to provide drugs blocking endothelin receptors within only a few years after the discovery of endothelin, it took more than 10 years for these drugs to reach the clinics. Initial clinical indications such as heart failure have been shown not to benefit from endothelin receptor blockade on top of standard treatment and are unlikely to ever become an indication for this new form of treatment. In contrast, a disease for which very strong preclinical evidence suggested therapeutic efficacy of endothelin antagonists such as pulmonary arterial hypertension meanwhile has become the first clinical indications for this new class of drugs. Similarly, results from basic science studies of diseases that are similarly associated with cell growth and/or inflammatory activation such as or resistant arterial hypertension and glomerulosclerosis or immune mediated disease such as cancer, connective tissue diseases, or chronic allograft rejection, or even metabolic diseases such as obesity or diabetes suggest that these conditions could become new indications for endothelin antagonist therapy in the near future. Well and carefully designed clinical studies are warranted to test and verify the therapeutic potential of this new class of drugs for cardiovascular medicine, nephrology, oncology and related medical fields.
(Adapted from Endothelin: 20 Years from Discovery to Therapy , Endothelin: 30 years from Discovery to Therapy, In memoriam: Paul M. Vanhoutte and The Discovery of Endothelium-Dependent Contraction: The Legacy of Paul M. Vanhoutte and updated 2019)
Further Reading
Bacon CR, Cary NR, Davenport AP.
Endothelin peptide and receptors in human atherosclerotic coronary artery and aorta.
Circ Res 1996;79:794-801.
Barton M, Yanagisawa M.
Endothelin: 20 years from discovery to therapy.
Can J Physiol Pharmacol 2008: 86:485-498
Barton M, Yanagisawa M.
Endothelin: 30 years from discovery to therapy.
Hypertension 2019: 74:1232-1265
Barton M, Kohan DE (editors)
Endothelin in renal physiology and disease
Contrib Nephrol 2011: 172: 1-266
Barton M.
The discovery of endothelium-dependent contraction: The legacy of Paul M. Vanhoutte
Pharmacol Res 2011; 63: 455-462
Barton M, Cardillo C.
In Memoriam: Paul M. Vanhoutte
J Physiol 2019; 597: 5761-5737
Baynash AG, Hosoda K, Giaid A, Richardson JA, Emoto N, Hammer RE, Yanagisawa M.
Interaction of endothelin-3 with endothelin-B receptor is essential for development of epidermal melanocytes and enteric neurons.
Cell 1994;79:1277-85
Benigni A, Zoja C, Corna D, Orisio S, Longaretti L, Bertani T, Remuzzi G.
A specific endothelin subtype A receptor antagonist protects against injury in renal disease progression.
Kidney Int 1993;44:440-444.
Benigni A, Remuzzi G. Endothelin antagonists.
Lancet 1999; 353(9147): 133-8
Clozel M, Breu V, Burri K, Cassal JM, Fischli W, Gray GA, Hirth G, Löffler BM, Müller M, Neidhart W, Ramuz H.
Pathophysiological role of endothelin revealed by the first orally active endothelin receptor antagonist.
Nature 1993; 365(6448):759-61.
de Nucci G, Thomas R, D'Orleans-Juste P, Antunes E, Walder C, Warner TD, Vane JR.
Pressor effects of circulating endothelin are limited by its removal in the pulmonary circulation and by the release of prostacyclin and endothelium-derived relaxing factor.
Proc Natl Acad Sci U S A 1988; 85: 9797-9800.
Davenport AP, Barton M.
Themed section: endothelin.
Br J Pharmacol 2013;168:279-82.
Davenport AP, Maguire JJ.
Of mice and men: advances in endothelin research and first antagonist gains FDA approval.
Trends Pharmacol Sci 2002;23:155-7.
Davenport AP, Hyndman KA, Dhaun N, Southan C, Kohan DE, Pollock JS, Pollock DM, Webb DJ, Maguire JJ.
Endothelin.
Pharmacol Rev 2016 68:357-418.
De Mey JG, Vanhoutte PM.
Heterogeneous behavior of the canine arterial and venous wall. Importance of the endothelium.
Circ Res 1982; 51:439-447
Emoto N, Yanagisawa M, Barton M
In memoriam: Tomoh Masaki
Hypertension 2020; 76:1664-1666
Furchgott, R.F.
Pharmacology of vascular smooth muscle.
Pharmacol Rev 1955; 7:183-265
Furchgott RF, Zawadzki JV.
The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine.
Nature 1980; 299:373–376.
Furchgott RF.
The discovery of endothelium-dependent relaxation.
Circulation 1993; 87 (Suppl.. V): V3-V8
Gillespie MN, Owasoyo JO, McMurtry IF, O’Brien RF.
Sustained coronary vasoconstriction provoked by a peptidergic substance released from endothelial cells in culture.
J Pharmacol Exp Ther.1986; 236: 339–343.
Goto K, Miyauchi T, Yanagisawa M.
Emergence of clinical applications of endothelin system inhibitors.
J Cardiovasc Pharmacol 2004;44 (Suppl 1): xiii-xiv.
Haynes WG, Hand MF, Johnstone HA, Padfield PL, Webb DJ.
Direct and sympathetically mediated venoconstriction in essential hypertension. Enhanced responses to endothelin-1.
J Clin Invest 1994; 94:1359-64.
Haynes WG, Webb DJ.
Contribution of endogenous generation of endothelin-1 to basal vascular tone.
Lancet 1994;344(8926):852-4.
Heerspink HJL, Parving HH, Andress DL, Bakris G, Correa-Rotter R, Hou FF, Kitzman DW, Kohan D, Makino H, McMurray JJV, Melnick JZ, Miller MG, Pergola PE, Perkovic V, Tobe S, Yi T, Wigderson M, de Zeeuw D; SONAR Committees and Investigators.
Atrasentan and renal events in patients with type 2 diabetes and chronic kidney disease (SONAR): a double-blind, randomised, placebo-controlled trial.
Lancet 2019;393:1937-1947
Hickey KA, Rubanyi GM, Paul RJ, Highsmith RF.
Characterization of a coronary vasoconstrictor produced by cultured endothelial cells.
Am J Physiol 1985;248:C550–C556.
Hosoda K, Hammer RE, Richardson JA, Baynash AG, Cheung JC, Giaid A, Yanagisawa M.
Targeted and natural (piebald-lethal) mutations of endothelin-B receptor gene produce megacolon associated with spotted coat color in mice.
Cell 1994;79:1267-76.
Inoue A, Yanagisawa M, Kimura S, et al.
The human endothelin family: three structurally and pharmacologically distinct isopeptides predicted by three separate genes.
Proc Natl Acad Sci U S A 1989; 86: 2863–2867.
Kedzierski RM, Yanagisawa M.
Endothelin system: the double-edged sword in health and disease.
Annu Rev Pharmacol Toxicol 2001;41:851-76.
Kisanuki YY, Emoto N, Ohuchi T, Widyantoro B, Yagi K, Nakayama K, Kedzierski RM, Hammer RE, Yanagisawa H, Williams SC, Richardson JA, Suzuki T, Yanagisawa M.
Low blood pressure in endothelial cell-specific endothelin 1 knockout mice.
Hypertension 2010;56:121-8
Kiowski, W, Sutsch G, Hunziker P, Muller, P, Kim J, Oechslin E, Schmitt R, Jones R, Bertel O.
Evidence for endothelin-1-mediated vasoconstriction in severe chronic heart failure
Lancet 1995; 358: 732-6.
Kohan DE
Endothelin-1 and hypertension: from bench to bedside.
Curr Hypertens Rep 2008; 10:65-9.
Kohan DE, Cleland JG, Rubin LJ, Theodorescu D, Barton M.
Clinical trials with endothelin receptor antagonists: what went wrong and where can we improve?
Life Sci 2012;91:528-339
Maguire JJ, Davenport AP.
Endothelin@25 - new agonists, antagonists, inhibitors and emerging research frontiers: IUPHAR Review 12.
Br J Pharmacol 2014; 171:5555-5572.
Masaki T.
The discovery of endothelins.
Cardiovasc Res 1998; 39:530–533.
O’Brien RF, Robbins RJ, McMurtry IF
Endothelial cells in culture produce a vasoconstrictor substance.
J Cell Physiol 1987; 132: 263–270.
Pollock DM.
Dissecting the complex physiology of endothelin: new lessons from genetic models.
Hypertension 2010;56:31-3.
Yang LL, Gros R, Kabir MG, Sadi A, Gotlieb AI, Husain M, Stewart DJ.
Conditional cardiac overexpression of endothelin-1 induces inflammation and dilated cardiomyopathy in mice.
Circulation 2004;109:255-61
Schneider MP, Boesen EI, Pollock DM.
Contrasting actions of endothelin ET(A) and ET(B) receptors in cardiovascular disease.
Annu Rev Pharmacol Toxicol 2007;47:731-59.
Stewart DJ, Kubac G, Costello KB, Cernacek P.
Increased plasma endothelin-1 in the early hours of acute myocardial infarction.
J Am Coll Cardiol 1991;18:38-43.
Toda N
The action of vasodilating drugs on isolated basilar, coronary and mesenteric arteries of the dog.
J Pharmacol Exp Ther 1974; 191:139-146
Vanhoutte PM
Inhibition by acetylcholine of adrenergic neurotransmission in vascular smooth muscle.
Circ Res 1974: 34:317-326
Vane JR, McGiff JC.
Possible contributions of endogenous prostaglandins to the control of blood pressure.
Circ Res 1975;36(6 Suppl 1):68-75.
Yanagisawa M, Kurihara H, Kimura S, Tomobe Y, Kobayashi M, Mitsui Y, Yazaki Y, Goto K. Masaki T.
A novel potent vasoconstrictor peptide produced by vascular endothelial cells.
Nature 1988;332:411–415.
Yanagisawa M, Inoue A, Ishikawa T, et al.
Primary structure, synthesis, and biological activity of rat endothelin, an endothelium-derived vasoconstrictor peptide.
Proc Natl Acad Sci U S A 1988; 85: 6964–6967.
